Psoriasis: a chronic skin disease
 Psoriasis is a chronic, genetic based, inflammatory disease that affects the skin causing swelling and flaking skin. It is not contagious but it can be inherited. Clinical history is highly diverse, with different degrees of evolution. It affects 2% of the world’s population (mostly Caucasian) and can develop at any age appearing in 75% of cases before 40 years old. Its etiology is multifactorial although an alteration of the immune system is present. Some factors closely linked to psoriatic outbreaks are:
Psoriasis is a chronic, genetic based, inflammatory disease that affects the skin causing swelling and flaking skin. It is not contagious but it can be inherited. Clinical history is highly diverse, with different degrees of evolution. It affects 2% of the world’s population (mostly Caucasian) and can develop at any age appearing in 75% of cases before 40 years old. Its etiology is multifactorial although an alteration of the immune system is present. Some factors closely linked to psoriatic outbreaks are:
- Biological factors (infections).
- Chemical factors (There are almost a hundred medicines that favour its appearance such as antibiotics, NSAID, beta-blockers, Psychotropics, etc.).
- Climatic factors (the cold aggravates psoriasis).
- Stress.
- Physical factors (Koebner’s phenomenon).
The diagnosis is primarily based on clinical history and secondarily on serology and skin biopsy. Psoriasis manifests itself clinically in different ways:
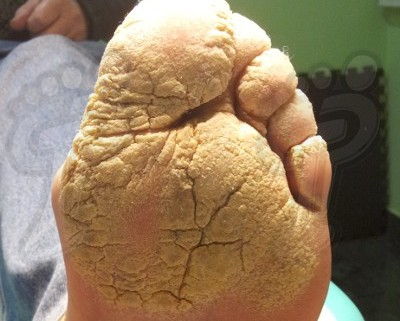
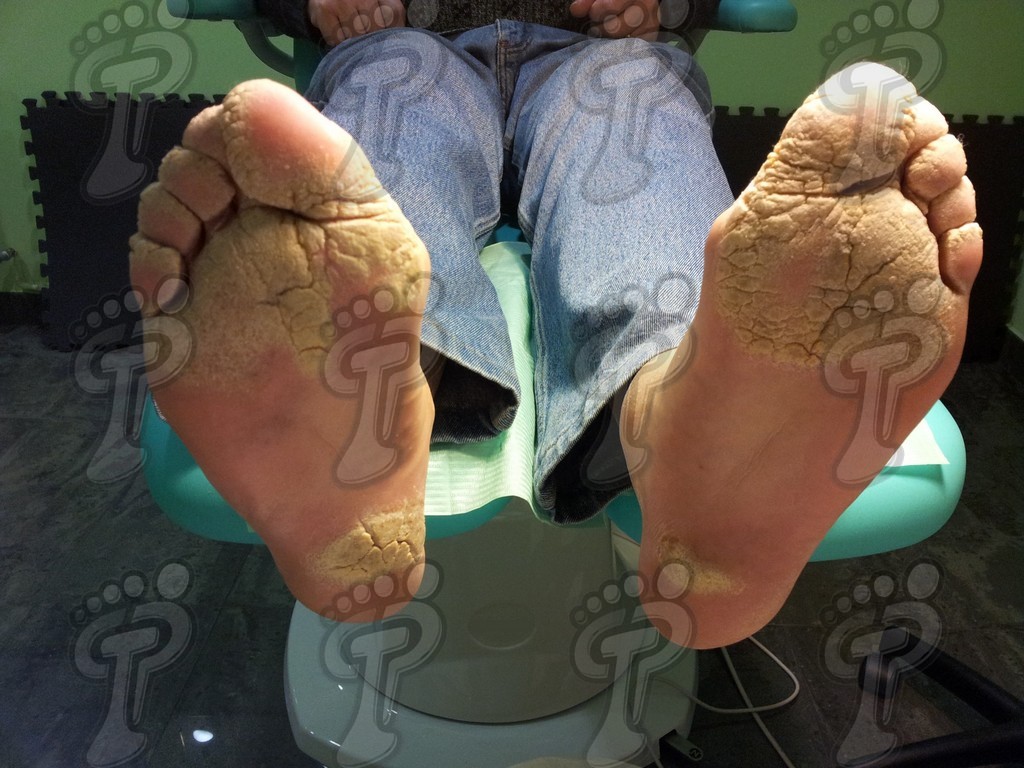
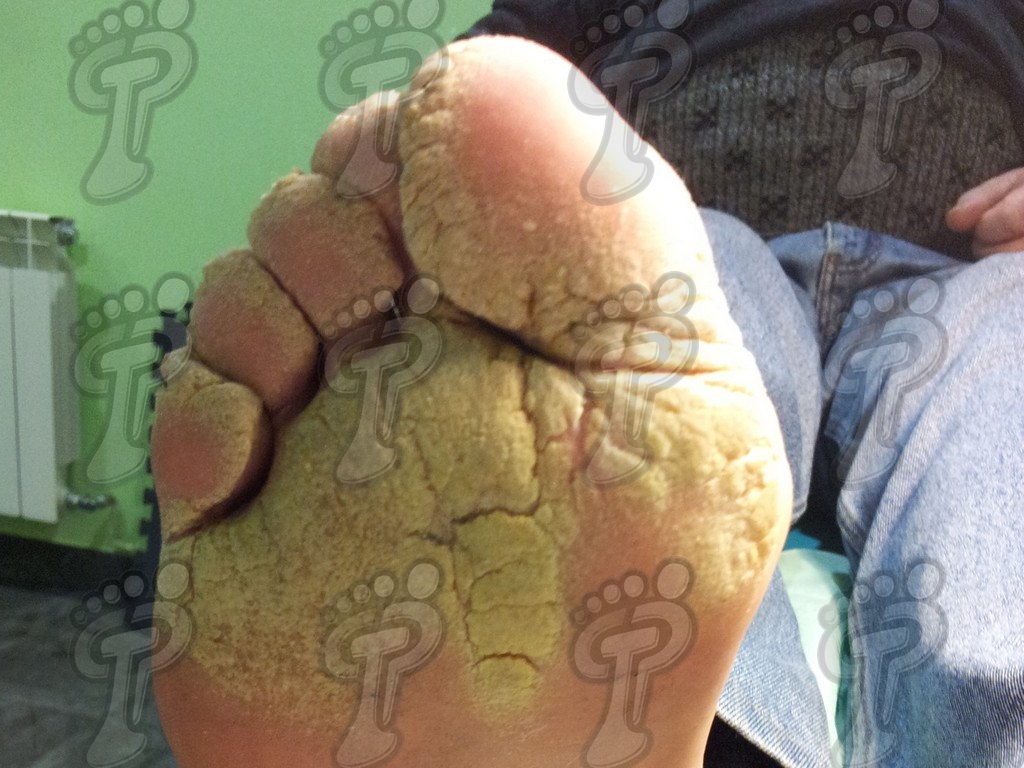
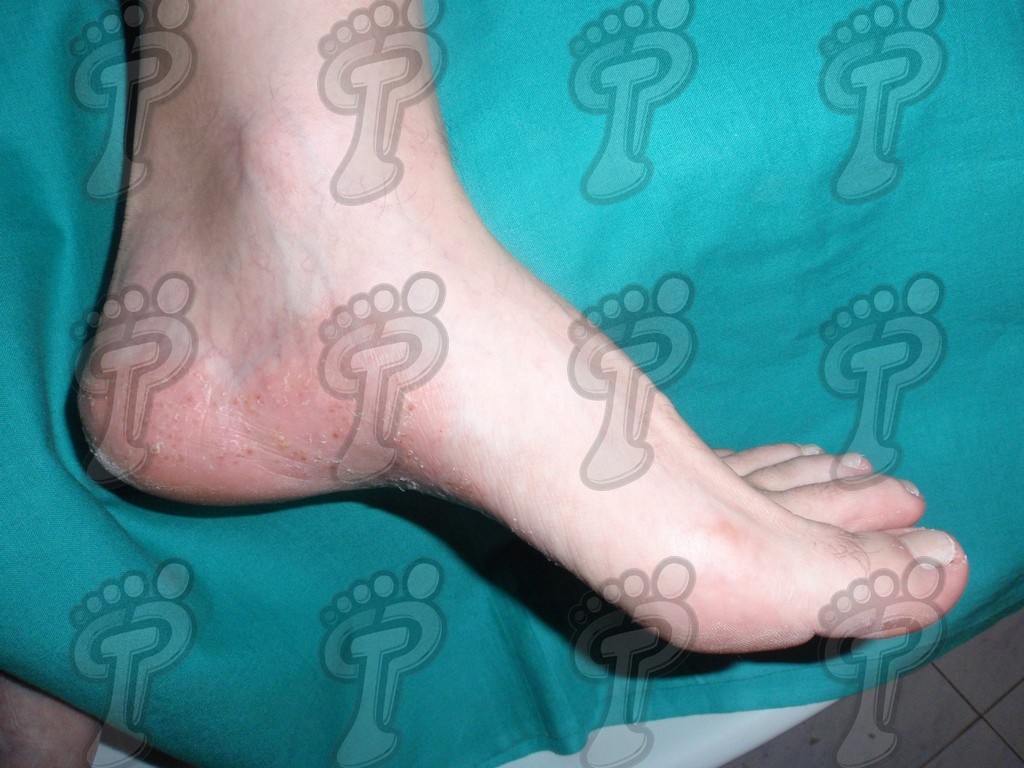
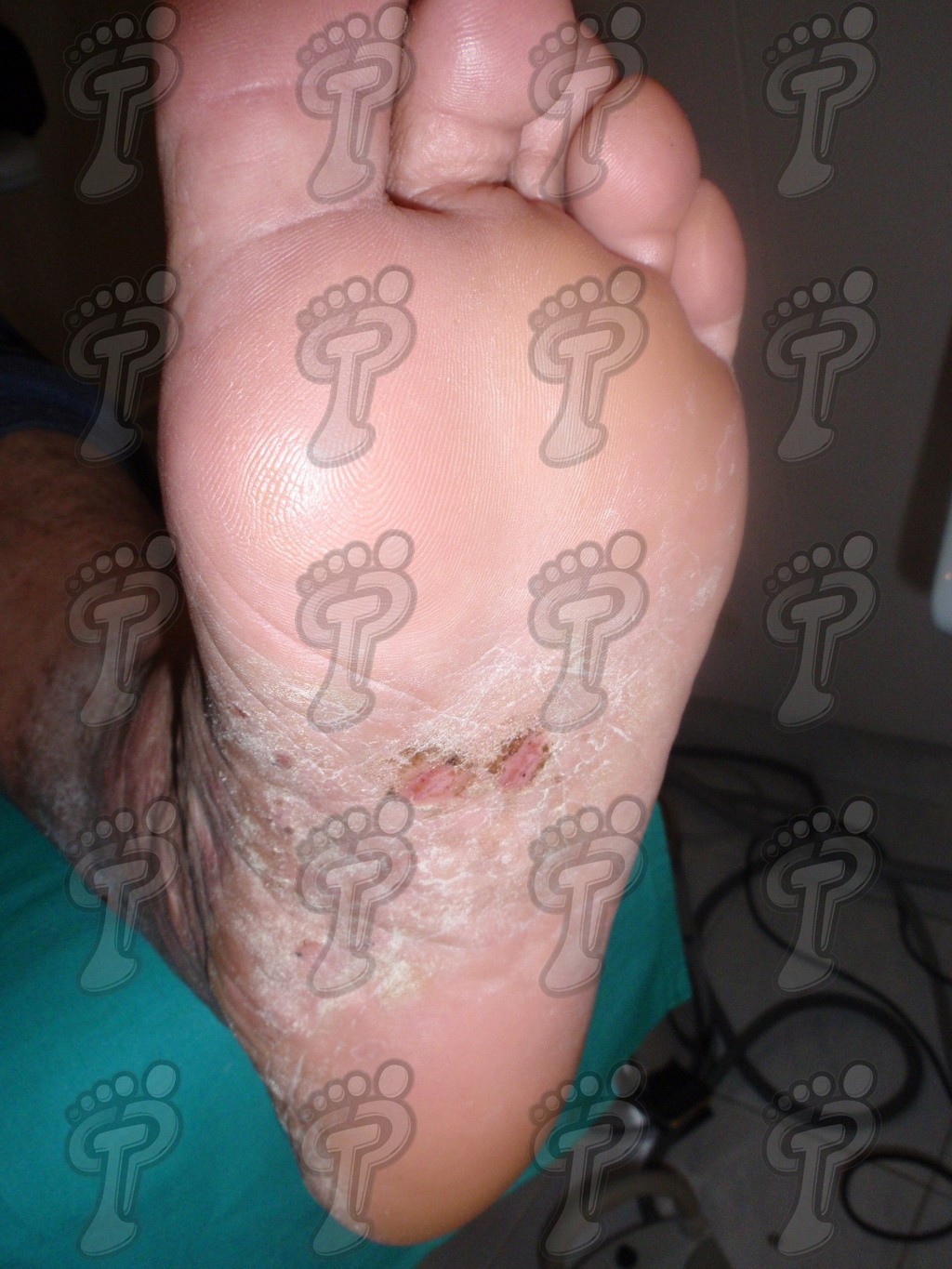
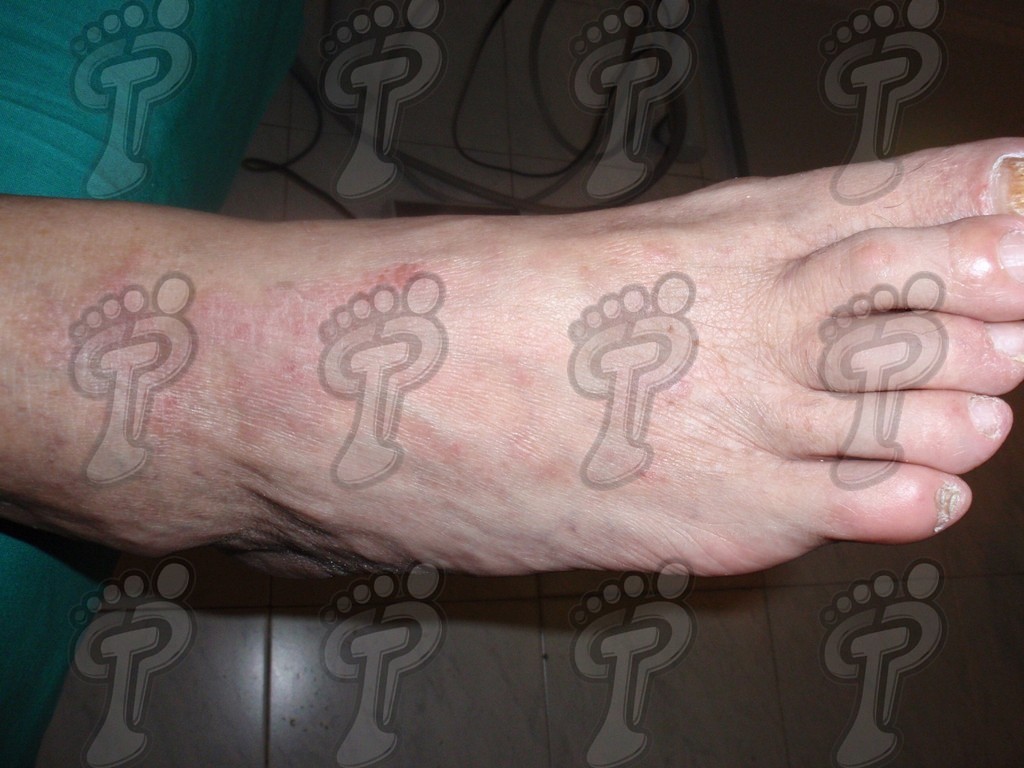
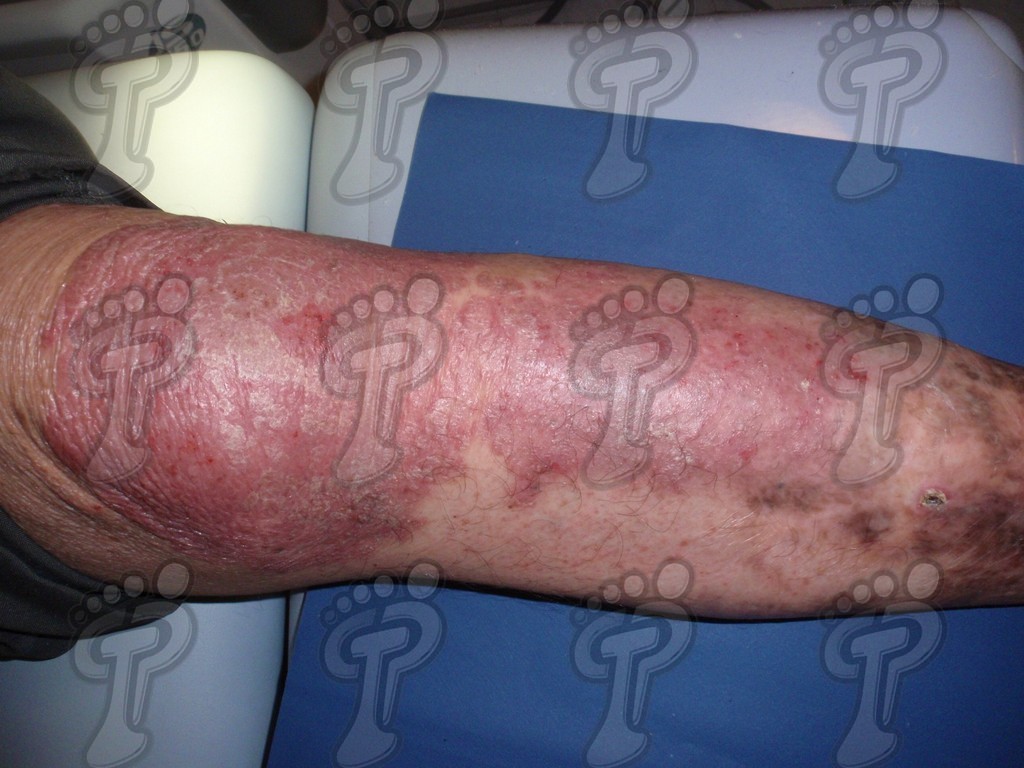
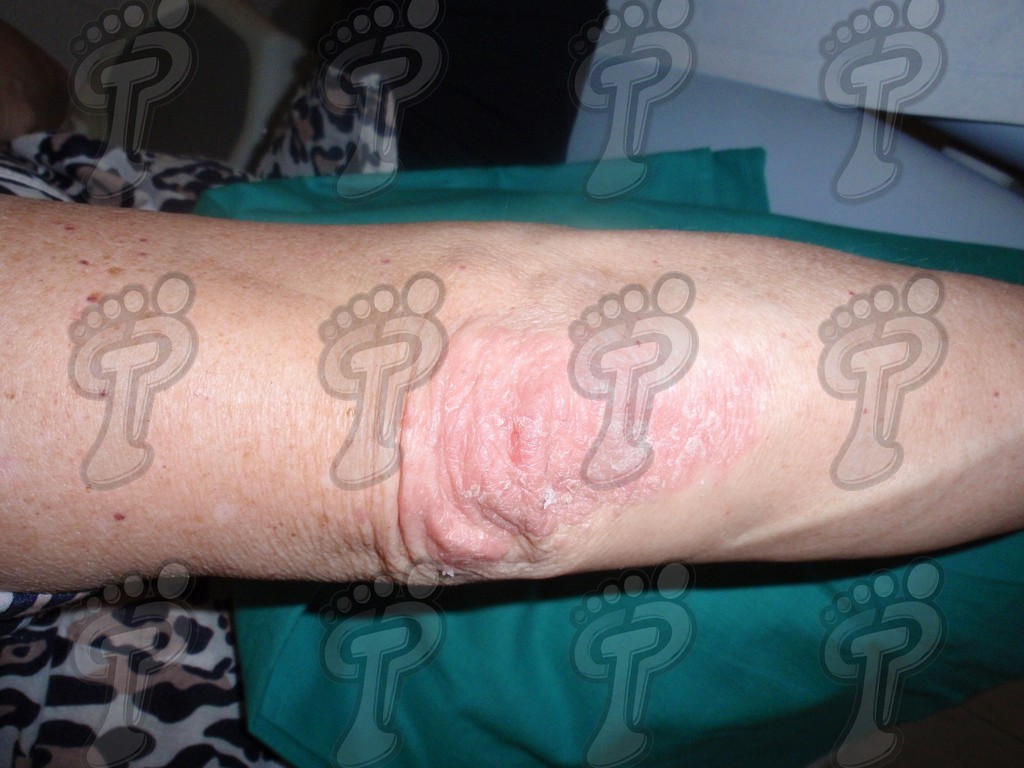
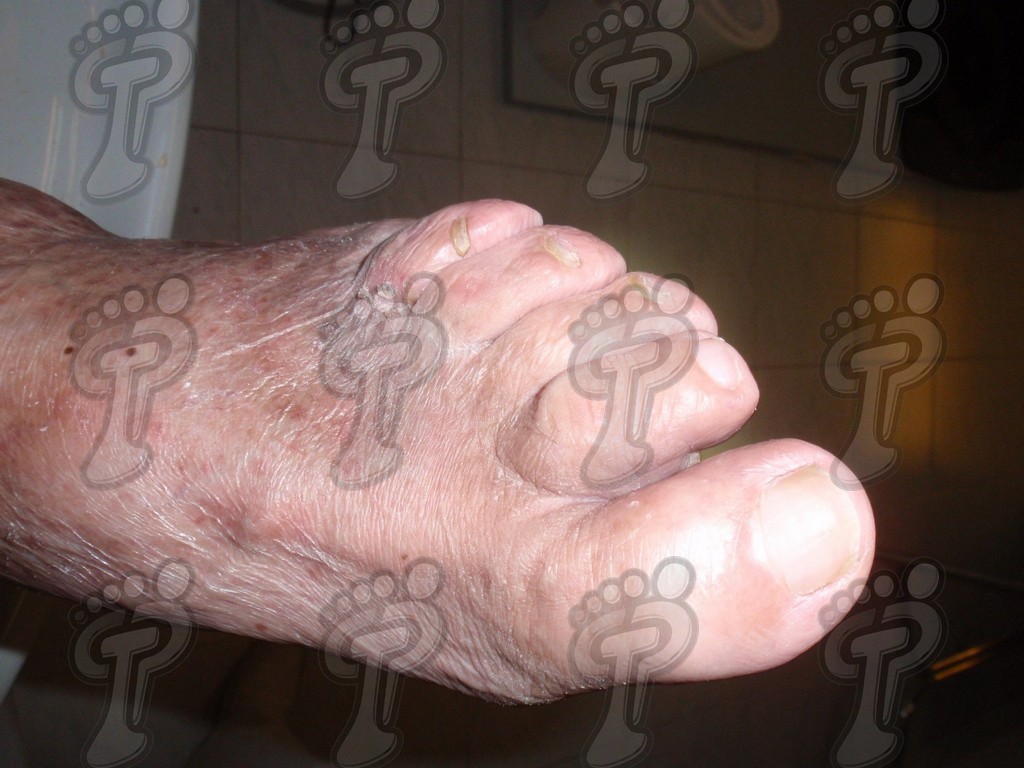
- Plaque psoriasis. It is the most common and is usually symmetrical. It basically affects hands, feet, elbows, knees and scalp. These patients often suffer:
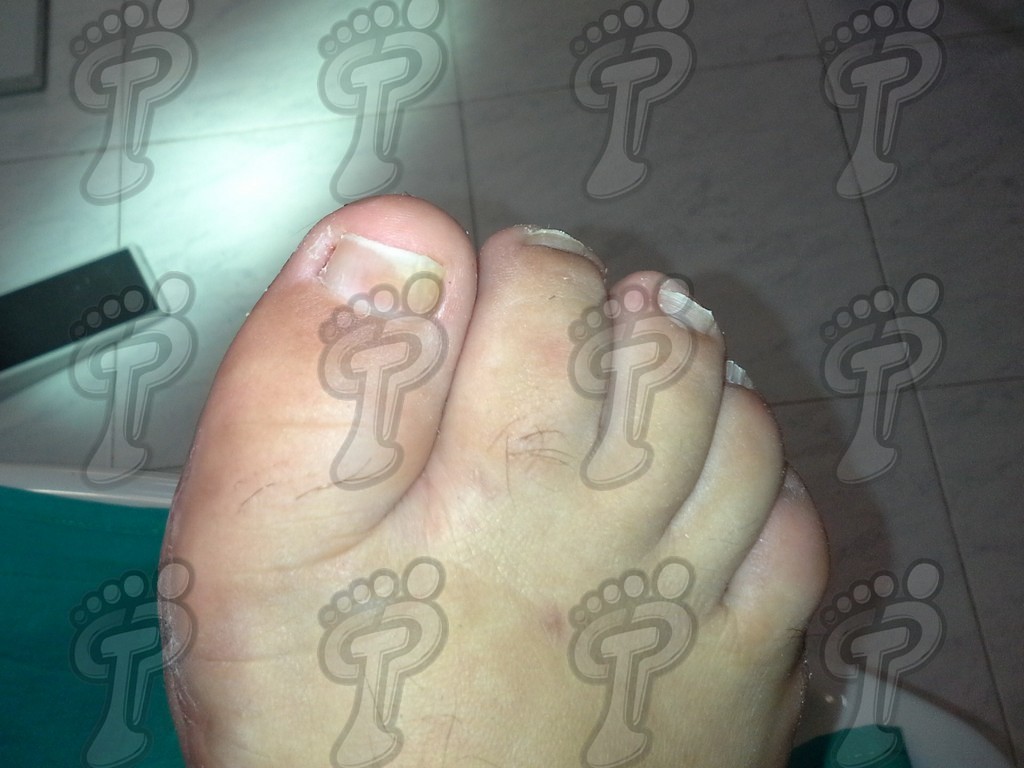
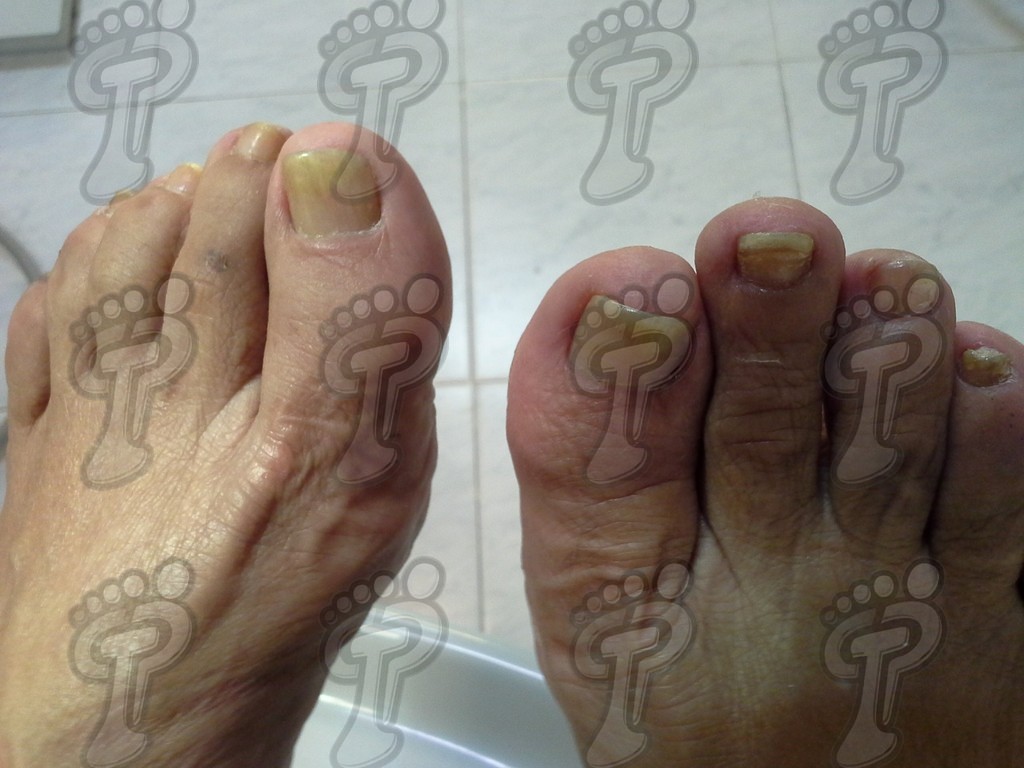
- Changes in nails such as onychodystrophy (due to the affection of the nail bed), oil stains due to alteration of the hyponychium, pitting (pitted nails), onycholysis (nail separates from the nail bed) and subungual hyperkeratosis.
- Pain.
- Itching.
- Fear of social rejection.
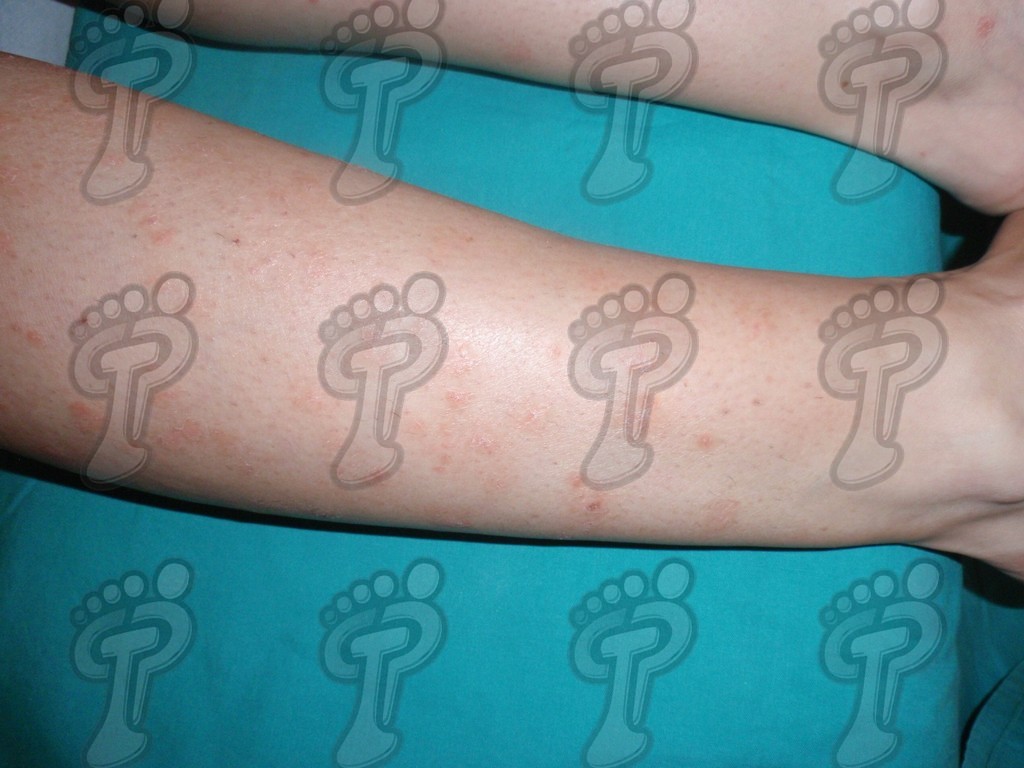
- Guttate Psoriasis. Numerous papules of approximately one centimeter in diameter appear due to a streptococcic infection (strep). It is more common in children.
- Localised pustular psoriasis. It presents itself with pustules on erythematous plaques, increased ESR, fever and leucocytosis.
- Psoriatic erythroderma. Together with pustular psoriasis it is a severe form of psoriasis that converts most of the patient’s skin in erythematous desquamative plaques. It usually occurs in systemic infections, phototoxicity and in discontinuing treatment with corticosteroids.
- Linear psoriasis.
- Inverse psoriasis.
Psoriatic arthropathy is a complication of psoriasis presenting an autoimmune inflammation of the joints. Mild forms of psoriasis are usually treated with topical therapies such as:
- Emollients.
- Keratolytics (salicylic acid, lactic acid, urea, etc.).
- Anthralins.
- Derivatives of vitamin D..
- Coal tar.
Severe states of psoriasis need the application of systemic treatments such as:
- Photochemotherapy.
- Phototherapy.
- Retinoids.
- Cyclosporine A.
- Methotrexate.







Leave a Reply
Want to join the discussion?Feel free to contribute!