SCARF TECHNIQUE FOR THE TREATMENT OF HALLUX VALGUS
The Scarf technique or in inverted Z is nowadays one of the most used techniques for the correction of the well-known “bunions”. The reason this technique is one of the most used is because of the great number of advantages this osteotomy provides:
- Moderate – severe Hallux Valgus (intermetatarsal angle between 12º – 20º).
- Pain as a reason for the first visit.
- Enough osseous quality to support osteotomies and synthesis.
- Well-kept articular state (the metatarsophalangeal joint doesn’t have arthrosis) and with possibilities of being improved after the articular reorientation.
- Osteotomy with a good intrinsic stability which allows the patient to put weight on his foot from the outset. The movement of the osteotomy avoids the key points of blood supply that reach the metatarsal.
The complications this technique has are:
- Avascular necrosis from the head of first metatarsal.
- Pseudarthrosis.
- Fracture of first metatarsal.
- Troughing effect with elevation.
- Infection.
- Hypocorrection (the most common).
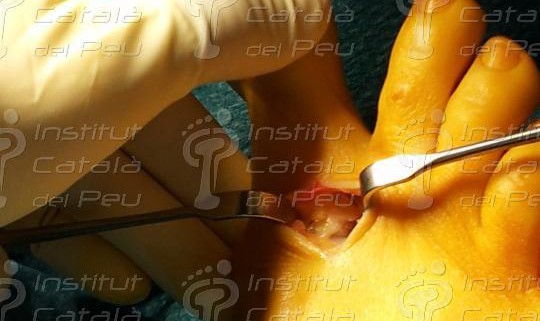
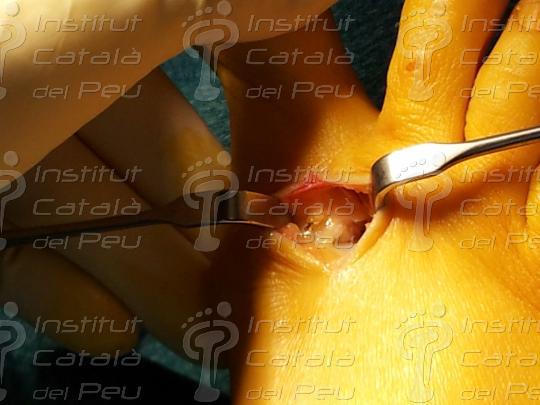
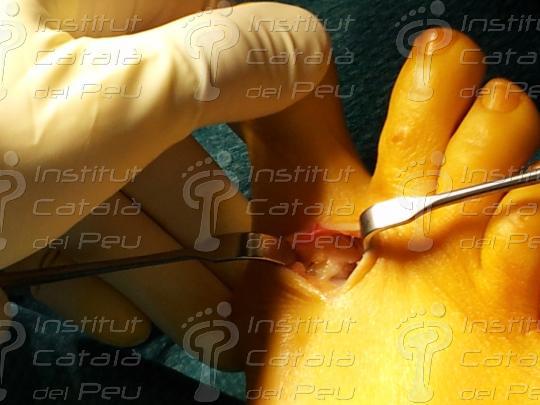
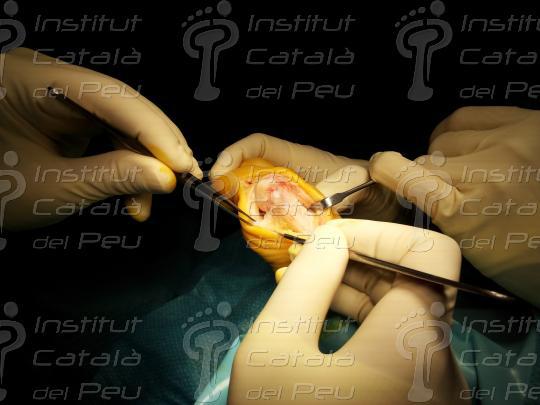
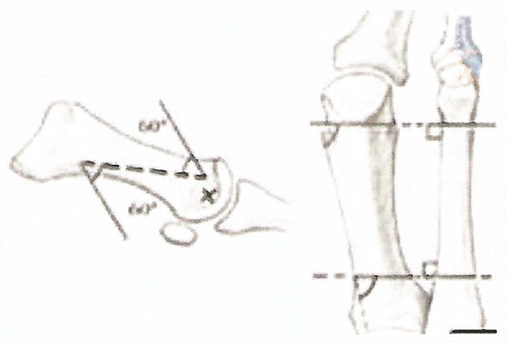
Once the capsulotomy and the bunionectomy have been made, the performance of this technique consists of making a longitudinal cut in the diaphysis of the metatarsal from the distal-dorsal to the proximal-plantar, this inclination of the cut to plantar being very important because it will allow the fall of the metatarsal head. To perform this cut we use as a guide two Kirschnner needles laid parallel to the axis of the floor and not to the axis of the metaldiaphysis. The Scarf technique or in inverted Z, is nowdays, one of the most used techniques for the correction of the so-called bunions. The reason this technique is one of the most used is because of the great number of advantages this osteotometatarsal has. When this cut is made, we make another dorsal distal cut and another proximal plantar cut, both of which are parallel and with a 60º angle.
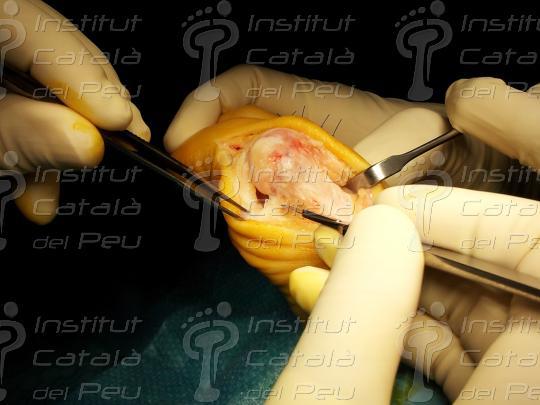
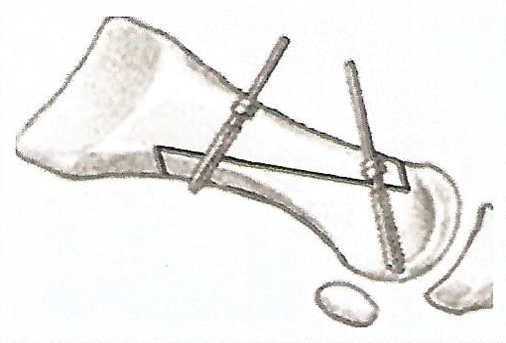
When we get to this stage, we can move the cephalic fragment to decrease the intermetatarsal angle. The displacement can be up to three quarters of the metatarsal surface. When we have got the result we want, we only have to fix the osteotomies with the chosen osteosynthesis. This is usually with two parallel screws and perpendicular to the diaphysis or one proximal, from dorsal to plantar, perpendicular to the diaphysis and the another pointing towards the distal with an inclination of 45ºa and which finishes in the metatarsal head.
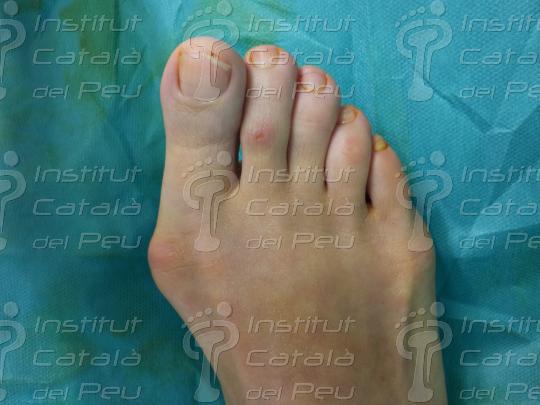
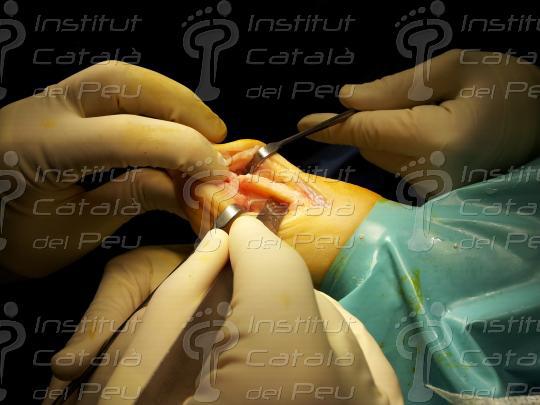
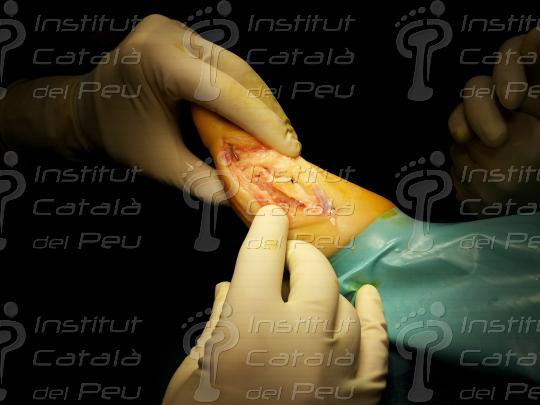
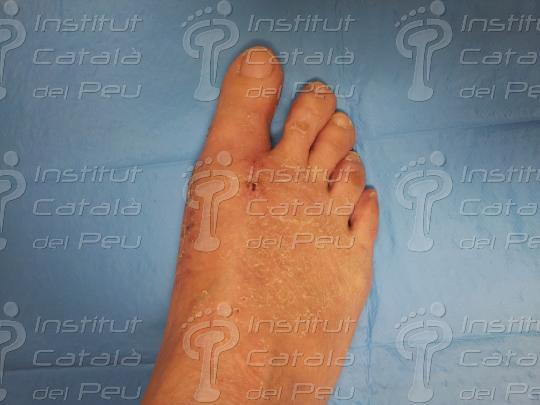
When the osteotomy is fixed in place, we resect the remains of the bone in the medial zone as a consequence of the metatarsal displacement. Finally, we suture the incisions by planes and we make a crossbreed bandage of the front part of the foot.






Leave a Reply
Want to join the discussion?Feel free to contribute!