RECONSTRUCTION OF THE ACHILLES TENDON. KEY ASPECTS OF SURGERY
The Achilles tendon joins the soleus muscle and the gemellus to the calcaneal bone and its main function is the elevation of the heel of the foot from the ground. It is the thickest and strongest tendon in our body and it inserts in the lower area by an anchorage to the calcaneal bone. It usually ploughs up two or three centimeters above the insertion due to a lack of vascularization.
When teasing or breaking the Achilles tendon, it is usually accompanied by the perception of a click or cracking, difficulty to stand on tiptoe, difficulty when wandering around or climbing the stairs, and ankle pain. In many times, there are previous cases of chronic tendinitis of the Achilles tendon or having been treated with antibiotics derived from quinolones.
The causes are traumatic (different kinds of accidents), sometimes at the beginning of a race, mainly on a tough ground, practicing sports in which the foot brakes or has sudden turns, or by the existence of clawfoot.
This kind of lesion may be diagnosed through a medical examination using the Thomson’s maneuver, but the use of magnetic resonance will be necessary in order to know deeply the existence when breaking the Achilles tendon.
A complete breaking of the Achilles tendon will need a surgical treatment, while in a partial fracture of the Achilles tendon will be necessary to value a restoring surgery of the use of a plaster during three or six weeks in order to regenerate the tendon (this plaster should be changed every two or three weeks to be able to stretch the Achilles tendon). The advantage of the surgery treatment is a low figure of recidivations in the fracture of the tendon, on the flip side, the disadvantage are the postoperative complications of any surgical wound.
The anesthesia which is realized in this kind of surgeries may be the epidural (relaxing the legs by the spinal anesthesia) or a general anesthesia of the patient.
The surgery begins with an approximately eight centimeters long incision from the calf to the ankle. The anatomical planes are separated until reaching the two ends of the torn Achilles tendon. Once it is delimited, the plantar thin muscle is located and it will be used as a graft and reinforcement of the suture of the Achilles tendon. After suturing the Achilles tendon, the plantar thin muscle tendon is used in a bow way between the two ends of the Achilles tendon. The next stage is to suture itself this bow to the Achilles tendon with biodegradable material.
It is important to protect the reconstructed Achilles tendon through its own physiological covering (paratenon) or with the support of some special dressing which avoids the adherences of the Achilles tendon to the skin. Finally, the anatomical planes of the skin are sutured.
The use of a drainage during one or two days is common to avoid the accumulation of hematic rests in the wound because they can cause complications in the correct cicatrization of the tissue.
In the postoperative stage it is necessary the use of crutches to walk because it is not possible for the leg to lean on the ground.
The angle between the foot and the leg should be 90º and with a plaster splint in order to avoid the rigidity of the ankle during the first two weeks.
The wandering around usually begins from the third week using a walker orthesis until the sixth week of the postoperative stage.
Once the patient is discharged, it should be recommended the use of orthopedic insoles to make the Achilles tendon be relaxed.
If progress is correct, a sportsman can run again from ten weeks after the postoperative stage.
It should be advisable to those patients who have had a fractured Achilles tendon to practice stretchings before getting exercise, as well as to avoid high-heeled shoes.

Fractured Achilles tendon
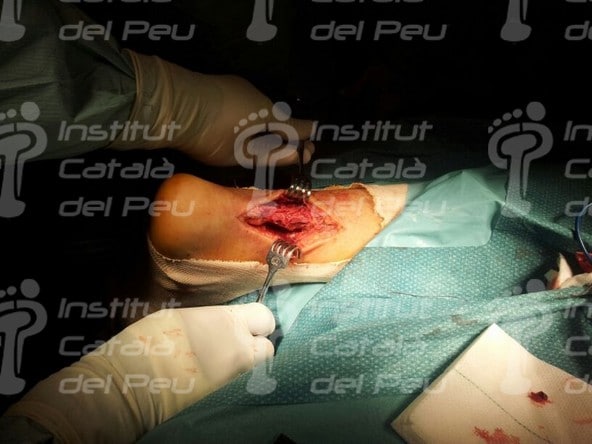
Fractured Achilles tendon
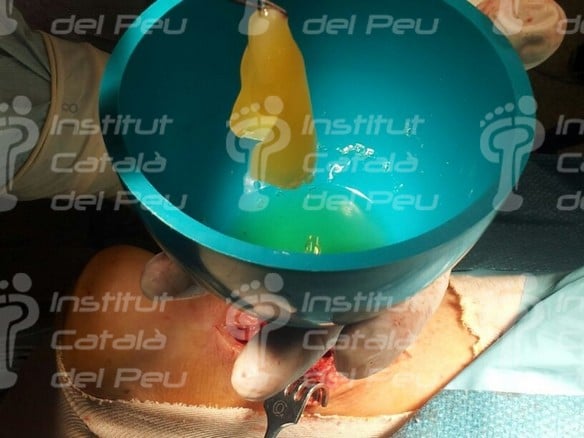
Fractured Achilles tendon
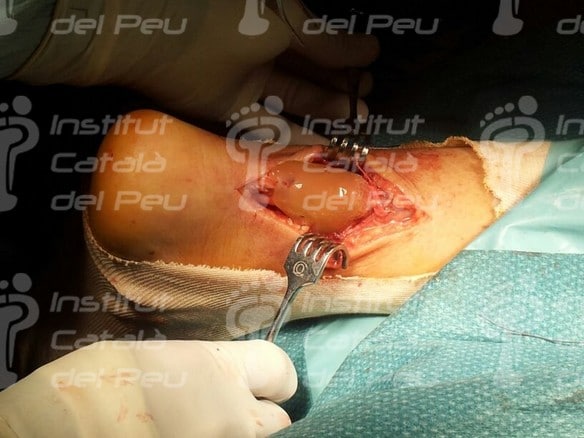
Fractured Achilles tendon
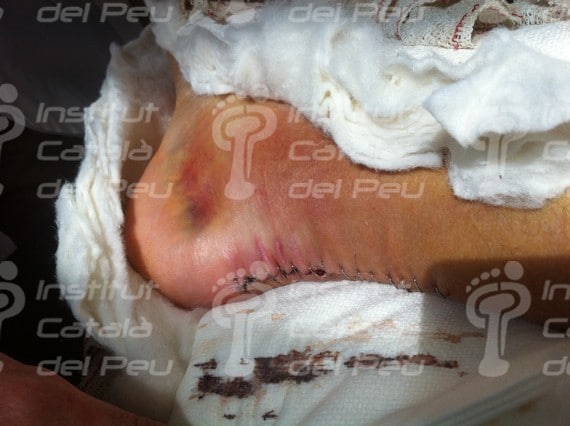
Fractured Achilles tendon
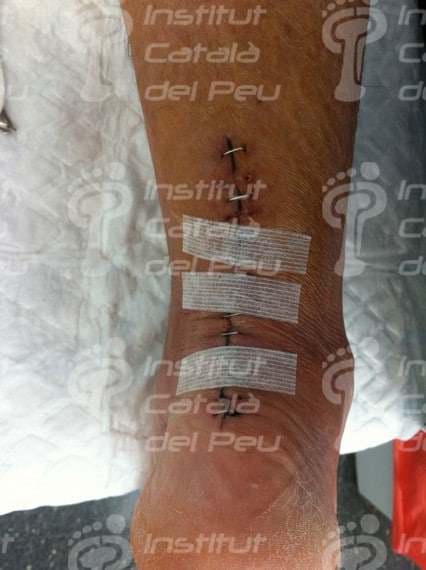
Fractured Achilles tendon
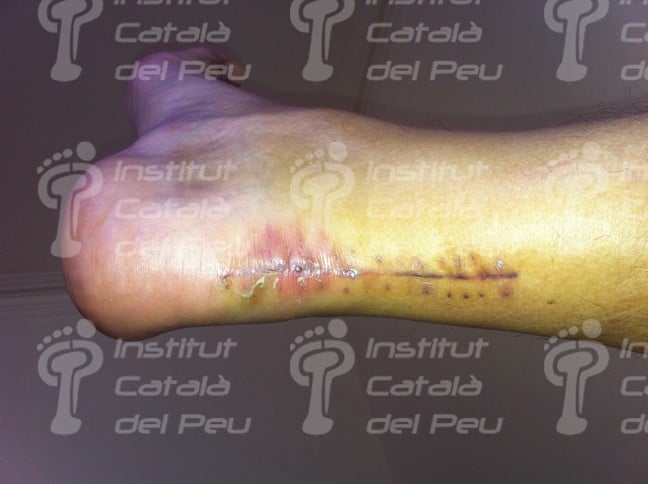
Fractured Achilles tendon
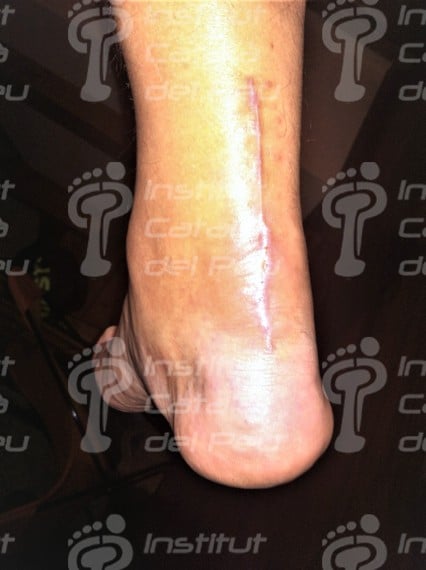
Fractured Achilles tendon








Leave a Reply
Want to join the discussion?Feel free to contribute!