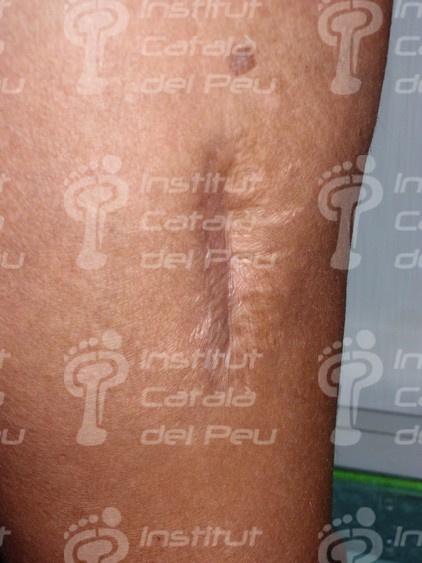
Scar is a permanent dermic disturbance as a consequence of a lesion and its repair. It is made of fibrous tissue which replaces the loss of tissue and which joins injured structures.
There are four stages in the cicatrisation process:
1- Inflammatory stage. Increase in vascularisation and therefore the platelets, thus helping the closure of the injury.
2- Proliferative stage. Collagen and fibrin are accumulated regenerating and tensing the injury.
3- Remodelling stage. Collagen is reabsorbed and it increases the tensile strength. It is the longest stage of cicatrisation.
4- Contraction stage. The injury’s bleeding surface area decreases with the concentric reduction of its size.
The factors that stimulate the growth of the cicatricial tissue are:
- Acute treatment. Closure of the injury without tension, control of the infection and debridement of the injury.
- Age. Scar hypertrophy risk is most common among young people.
- The depth of the injury.
- The kind of skin. Red-haired people have a very high probability, followed by people with dark skin.
- Malnutrition.
- Alcoholism and nicotine poisoning.
Scars can have cosmetic and functional problems for the patient.
Scars are broken down into five categories:
- Hypopigmented scar. The scar has a lighter colour than the rest of the skin because of the disability to produce melanin in this area due to the traumatism caused.
- Hyperpigmented scar. The scar is darker and it appears in superficial scars. It is a consequence of a bigger degree of melanogenesis together with the inflammatory reparative process.
- Hypertrophic scars.
- Keloid scars.
- Other types of scars, such as, retractile scars, atrophic scars, etc. This kind of scar is slightly sunken with respect to the surface of the skin for lack of enough tissue to cover thewound. It is typical of acne or chicken pox.
Hypertrophic scars are located in the traumatic area of the initial injury without invading the adjacent tissues. Their growth starts after the closure of the wound and it can continue to hypertrophy to 8 months. The causes are due to mechanical factors, early ages, infections of the injury, as well as the anatomical location.
Keloid scars cover beyond the initial injury as a consequence of the anomalous formation of collagen in order to revitalize the connective tissue after the lesion.
They are less common than hypertrophic scars. They start to grow at the beginning of a traumatism and they can continue to grow without a sign of stabilization for up to one year. These scars appear more frequently on people with dark skin, young women, pregnant women and in anatomical areas like the neck, shoulders, the lobe or the sternum area. They are a flesh-coloured tone, pink or red and they appear as a consequence of traumatisms, surgical injuries, burns, chicken pox, etc.
Keloid scars don’t usually improve spontaneously while hyperthophic scars can improve aesthetically without any treatment.
The most frequent treatments against keloid scars are radiotherapy, cryotherapy, laser treatment, infiltrations of corticosteroids that reduce the inflammation, as well as cosmetic surgery. We have to take into account that such treatments reduce the size of keloid scars, which do not disappear totally in most of the cases. The criteria of choosing one treatment or another will depend on the sort of scar while always considering the connection between the advantages and the risks.
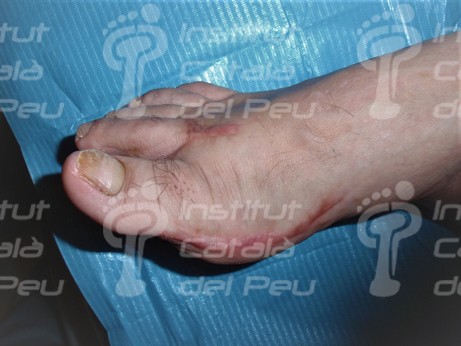
Hypertrophic scar caused by a hallux valgus operation.
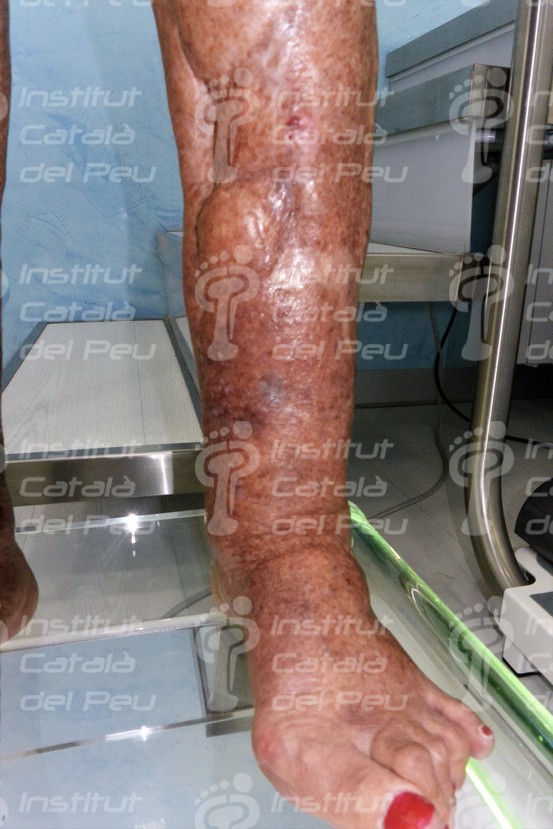
Hypertrophic scar caused by a traumatism.
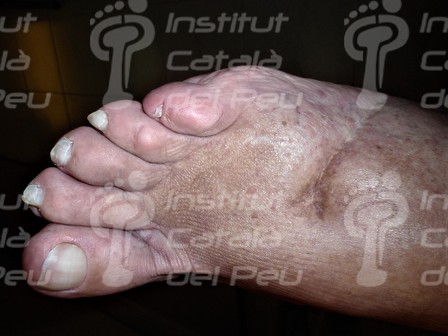
Hypertrophic scar caused by a traumatism.
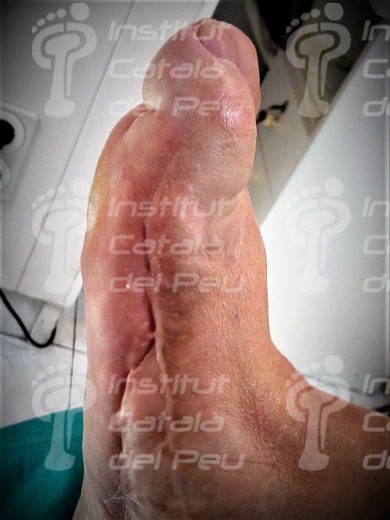
Post-surgery hypertrophic scar.
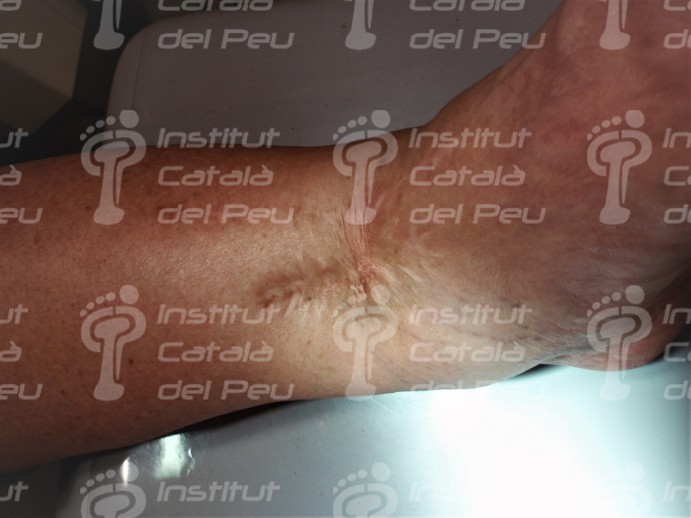
Hypertrophic scar.
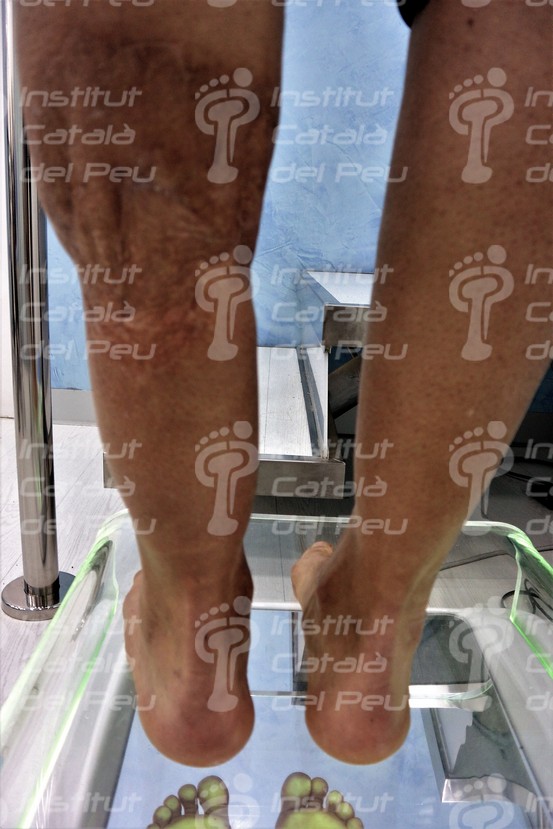
Hypertrophic scar caused by a traumatism.
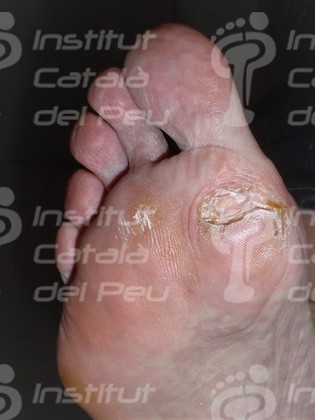
Plantar scar caused by self- injury when removing a callosity.
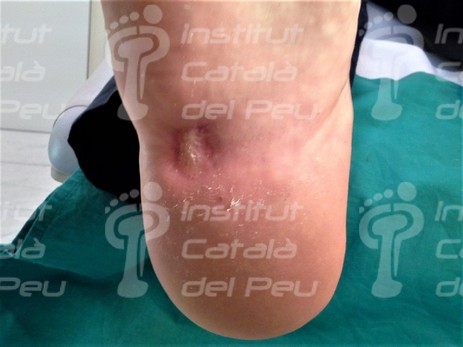
Post-surgery scar caused by benign tumour exeresis.
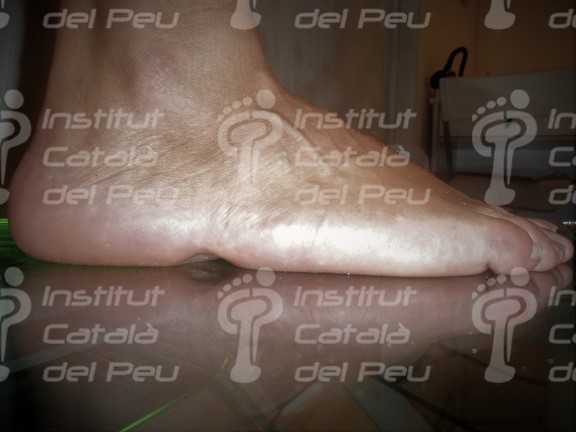
Same case with bipedestation. Observe the lack of adjacent tissue.
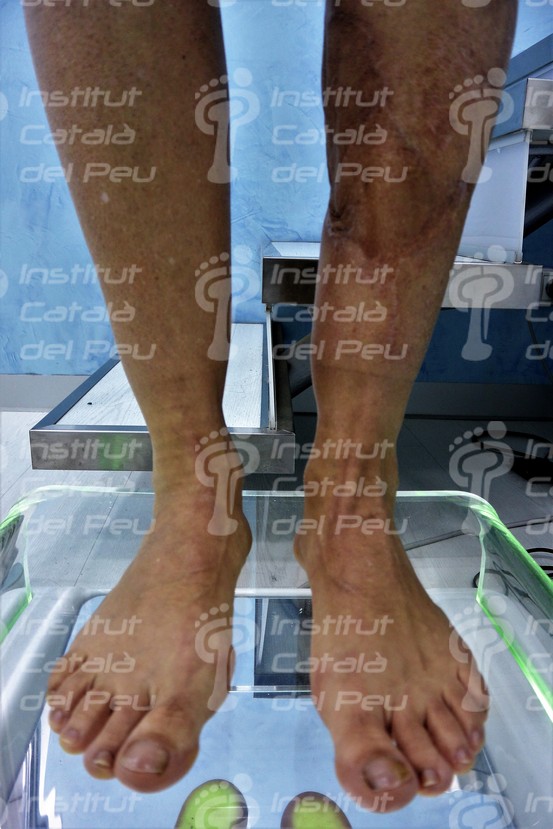
Keloid scar.